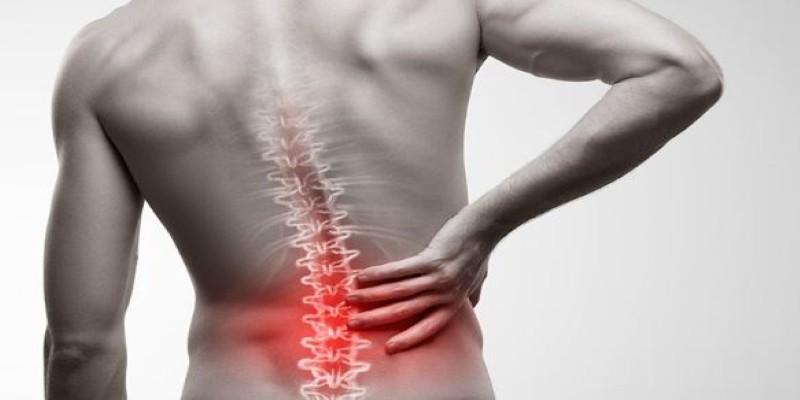
Back pain often appears during ordinary moments rather than accidents. A morning spent seated, an afternoon of household tasks, or a brief period of awkward movement can initiate symptoms that linger. Clinical records repeatedly link pain onset to routine physical demands that accumulate quietly across days and weeks. These patterns challenge assumptions that injury must involve a single clear event. Understanding how everyday activity interacts with spinal tissue helps explain delayed flares, uneven recovery, and recurring discomfort. This perspective clarifies why diagnostic timelines vary and why management plans focus on movement patterns, workload history, and tolerance instead of isolated incidents.
How Routine Movements Strain the Spine Over Time?
Daily movement keeps the spine healthy, yet repetition without enough change places quite a strain on supporting tissue. Sitting for long periods illustrates this well. Clinics regularly see back discomfort linked to desk routines rather than injury. Exams often show stiff hips, limited mid back motion, and delayed core engagement. Imaging may reveal mild disc drying or small bulges, changes tied to sustained flexed positions, and low muscle activity. Over time, tired muscles offload work onto joints and connective tissue. The result is stiffness when standing up or pain during the first bend of the day.

Lifting tasks at home tend to load the spine unevenly. Carrying shopping bags, moving boxes, or holding weight on one side shifts pressure across the lower back. During therapy assessments, asymmetry appears quickly. One side feels tighter, breathing becomes shallow, and bending relies too much on the lower spine instead of the hips. These patterns develop slowly and often go unnoticed until pain interrupts routine tasks.
Reaching and twisting add another layer of stress. Repeated overhead activity increases rotational demand at the junction between the upper and lower spine. Workplace evaluations often reveal limited trunk rotation paired with shoulder overuse, raising strain during chores. Imaging still has limits. Similar findings appear in people without pain, so care decisions depend on movement quality, symptom patterns, and daily load rather than scans alone.
Why Minor Stressors Can Lead to Pain Flares?
Pain flares often look sudden, yet the groundwork is usually laid over days. Repeated low-level strain leaves spinal and muscular tissue more reactive. Small inputs, a longer drive, a night of poor sleep, and an extra flight of stairs can then feel disproportionately sharp as irritated nerve endings fire sooner and longer. Clinicians in pain clinics hear this story after travel weekends or schedule changes, when normal pacing disappears.
Local inflammation can add fuel. Tiny stresses around facet joints, tendon insertions, or supporting ligaments promote swelling. Movement becomes guarded, not from damage alone, but from the body tightening to limit motion. Home-care staff commonly notice this during sit-to-stand transfers: the back stiffens, steps shorten, and reaching for a countertop triggers a protective spasm.
Timing creates confusion. Symptoms may peak the next morning or two days later, so the trigger gets missed, and activity swings between overdoing and complete rest. Short appointments rarely leave room to map these patterns in detail. Simple tracking, noting activity, sleep, and pain intensity, can reveal the build-up cycle, though follow-through is inconsistent.
Stress can amplify the loop. High workload and fragmented sleep raise muscle tone and lower pain thresholds, making minor mechanical strain feel like a major setback. Medication shifts can contribute, especially after missed doses.
Recovery Expectations in Clinical and Home Settings
Recovery after activity related back pain rarely moves in a clean upward line. Early gains can slow, then a busy day of errands or a long commute can bring symptoms back. Therapy teams plan for that. In outpatient rehab, weekly changes often reflect what the body tolerated, not a preset calendar. Better signs include smoother bending, less guarding after sitting, and longer standing time without a next day spike, rather than instant pain relief.
Pacing drives successful plans. Activity returns in small steps so irritated tissue can settle while strength rebuilds. Walking is commonly used since it loads the spine gently and keeps the hips moving. Sessions may start with short loops and a check the following morning for stiffness, sleep disruption, or leg symptoms.
Care looks different across settings. In hospital care, early mobilization prevents loss of conditioning and reduces fear of movement. In home care, the focus shifts to safer routines such as changing laundry height, adjusting bed entry, and placing frequently used items at waist level. Rest still has a place, yet prolonged inactivity weakens support muscles. Clear written plans and consistent follow up reduce stop start cycles.
Preventive Adjustments and Their Practical Limits
Preventive strategies often focus on managing how force moves through the spine during daily activity. Small ergonomic changes can alter stress patterns in meaningful ways. In workplace assessments, adjustments such as seat depth, desk height, or screen position frequently reduce prolonged spinal flexion. These changes tend to lower flare frequency across weeks rather than produce immediate relief, which can affect expectations.
Exercise based prevention adds another layer. Strength and flexibility programs aim to improve endurance in stabilizing muscles and maintain joint control during routine tasks. Clinical follow up shows progress depends less on exercise selection and more on regular completion. Adherence often declines once supervised sessions end, especially after pain decreases and urgency fades.
Task modification remains practical. Dividing household chores into shorter segments and alternating postures limits cumulative strain. Home care assessments commonly highlight these adjustments during functional reviews. Limits remain unavoidable. Degenerative changes, prior injuries, and overlapping conditions restrict the preventive impact. Risk reduction is realistic. Complete prevention is not.
Conclusion
Everyday activity influences back pain through repeated movement patterns, gradual posture changes, and uneven load exposure. Clinical care often uncovers links to routine habits rather than isolated incidents. Recovery tends to progress unevenly, shaped by pacing, careful evaluation, and time for tissue response. Imaging results may fail to explain symptom severity, and flare patterns differ widely. Recognizing these dynamics encourages more realistic planning, clearer communication, and safer choices across home care, outpatient treatment, and ongoing clinical follow up.